 SNF professionals have been eagerly awaiting the SNF PPS Proposed Rule due to be released any day now to see if significant changes will be made to what is expected to come October 1st, 2019 with the new Patient Driven Payment Model (PDPM).
SNF professionals have been eagerly awaiting the SNF PPS Proposed Rule due to be released any day now to see if significant changes will be made to what is expected to come October 1st, 2019 with the new Patient Driven Payment Model (PDPM).
Late yesterday afternoon (4/19/19) the 232 page Proposed Rule was released. Though this Rule proposes updates to multiple SNF areas of importance, the following information focuses on changes proposed for Group Therapy.
Current Rule for Group Therapy
Group Therapy for SNF Part A residents has been defined by the RAI Manual as “4 residents performing same or similar activities, regardless of payer source,” since 1998. In 2012, the word “exactly” was added to require exactly 4 residents in a group. Medicare Part B residents have always been the exception to this rule, as Medicare Part B requires coding Group Therapy when 2 or more residents are treated together for any reason.
Proposed Rule for Group Therapy
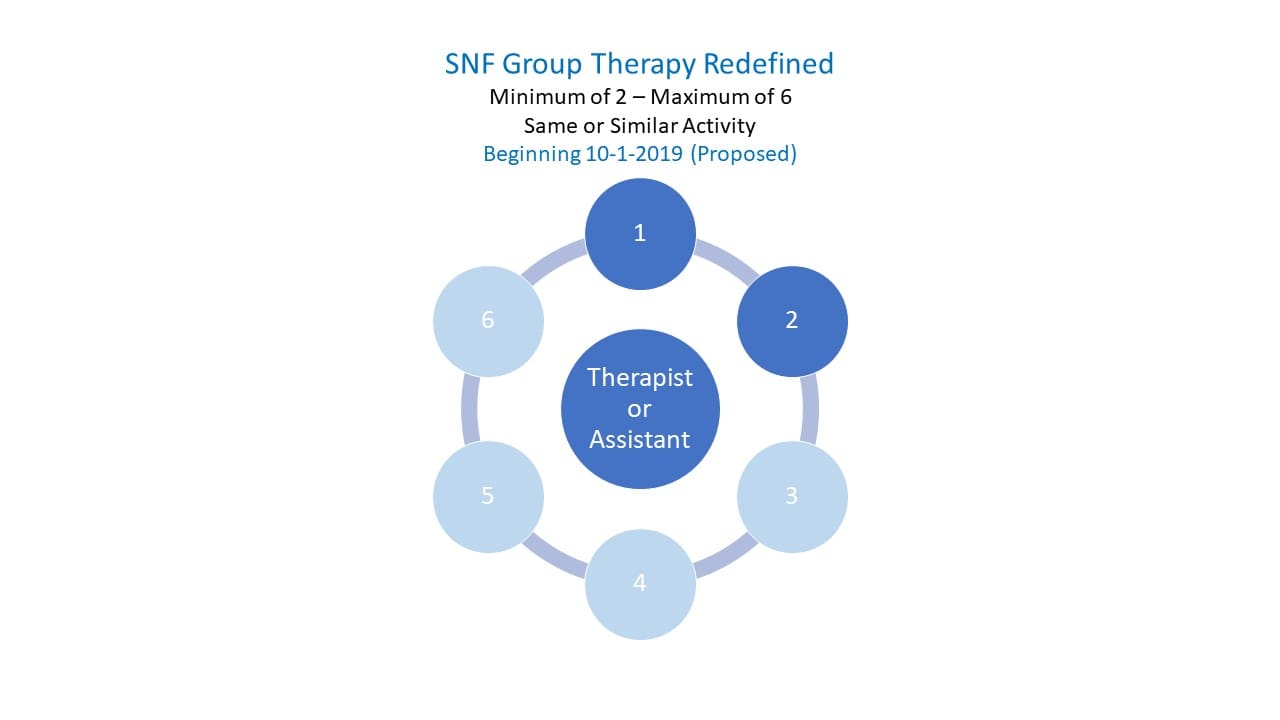
CMS is proposing a new definition for Group Therapy for use under PDPM effective October 1, 2019, as follows:
“Group Therapy in the SNF Part A setting will be defined as a qualified rehabilitation therapist or therapy assistant treating two to six patients at the same time who are performing the same or similar activities.”
CMS stated this definition mirrors the IRF (Inpatient Rehab) setting, and their plan to adopt this definition is part of an overall effort to increase consistency across Post Acute Care settings. CMS stated they believe this definition would offer therapists in the SNF “more clinical flexibility when determining the appropriate number for a group, without compromising the therapist’s ability to manage the group and the patient’s ability to interact effectively and benefit from group therapy.”
CMS looked at group therapy provision in the IRF and in the outpatient settings where the definition of group therapy is less restrictive than the current definition under the SNF PPS, and stated they “found that therapists do seem capable of managing groups of various sizes. Based on this review, we believe therapists have the clinical judgment to determine whether groups of different sizes would clinically benefit their patients, which they should be able to demonstrate with adequate documentation.”
CMS further states: “We continue to believe that individual therapy is the preferred mode of therapy provision and offers the most tailored service for patients. As we stated in the FY 2012 proposed rule (76 FR 26387), while group therapy can play an important role in SNF patient care, group therapy is not appropriate for either all patients or for all conditions, and is primarily effective as a supplement to individual therapy, which we maintain should be considered the primary therapy mode and standard of care in therapy services provided to SNF residents.”
In the Proposed Rule, CMS comments on specific group examples:
Patients can often benefit from the psycho-social aspect of groups, and in some situations, a group of six participants is not too large to provide that benefit to participants. For example, a cooking activity which will provide very functional therapy for patients planning to return home can be done in a group of six that will enhance the patient’s psycho-social experience in the SNF. Alternatively, a group of 2-3 patients can be clinically useful for certain patients as well. For example, a group of 2-3 patients who have pragmatic language difficulties following a stroke or head injury could very well benefit from a small communication group to work on the social aspects of language together without the concern of distraction that a larger group might cause. Thus, while we continue to maintain minimal concerns that some groups may be either too small or too large to allow for effective interaction, we believe that the potential clinical benefits of various size groups outweigh our concerns, and that it would be appropriate to allow therapists greater flexibility to perform therapy in groups of different sizes.
What Is Not Changing
This proposal does NOT change the 25% limit on combined Group and Concurrent Therapy for each discipline, and CMS goes one step further in the Rule to state:
“We continue to maintain that when group therapy is used in a SNF, therapists must document its use in order to demonstrate why it is the most appropriate mode of therapy for the patient who is receiving it. Group therapy is not appropriate for either all patients or all conditions, and in order to verify that group therapy is medically necessary and appropriate to the needs of each beneficiary, SNFs should include in the patient’s plan of care an explicit justification for the use of group, rather than individual or concurrent, therapy. This description should include, but need not be limited to, the specific benefits to that particular patient of including the documented type and amount of group therapy; that is, how the prescribed type and amount of group therapy will meet the patient’s needs and assist the patient in reaching the documented goals.”
What Does This Mean for SNF Therapy Professionals?
The individual resident’s need for Group Therapy should be determined by the evaluating therapist. CMS has made this very clear. A cookie-cutter approach to adding Group Therapy for every resident in every Plan of Care clearly defies everything CMS has documented above. CMS’s intent is to keep the power of clinical decision making with the clinician. As such, corporate mandates for group (and concurrent) therapy should be questioned. It is the individual clinician that is required to provide documentation to justify the medical necessity for these services.
This new definition of Group will require therapists to pay close attention to coding. Because the minimum limit is now 2 residents, therapists will need to be able to clearly identify if 2 residents treated at the same time is “Group” or “Concurrent,” and code accordingly. For example, 2 Part A residents treated at the same time by 1 therapist would be coded as “concurrent” if they were performing different activities, and coded as “group” if they were performing similar activities. Concurrent and group treatments should both be “pre-planned” events, so the intent of the treatment should be clear from the start. However, coding a treatment for 2 Part A residents as “group” will be something new for all therapists and will require a new mindset.
Important Links
Here are the important links if you would like to explore the Proposed Rule further:
SNF PPS Proposed Rule for FY2020
Remember, the Proposed Rule allows for providers to comment on all the provisions, which CMS will take into consideration prior to the release of the “Final Rule” in August. CMS encourages comments and thoughts on this proposed rule and will accept comments until June 18, 2019. The proposed rule [CMS-1718-P] can be downloaded from the Federal Register at: https://www.federalregister.gov/documents/2019/04/25/2019-08108/medicare-program-prospective-payment-system-and-consolidated-billing-for-skilled-nursing-facilities. Instructions on how and where to direct comments can be found on the third page of the PDF.
If you have any questions, send them to our Just Ask Q&A Forum and we will respond to you individually.
In your corner,
Dolores
Dolores Montero, PT, DPT, GCS, RAC-CT
SNF Therapy & MDS Compliance
